Dental implant technology and innovations are revolutionising the way we restore smiles, with groundbreaking advancements that promise faster healing, better success rates, and more comfortable procedures.
These cutting-edge developments are transforming what’s possible in implant dentistry, but which innovations are truly changing the game in 2024?
What Are the Latest Innovations in Dental Implant Technology?
The latest dental implant innovations in 2024 include AI-guided surgery systems, smart implants with integrated biosensors, 3D-printed custom implants, and advanced bioactive materials. These technologies achieve 98% success rates through precise computer-guided placement, nanostructured surfaces for enhanced osseointegration, and minimallyinvasive protocols that reduce healing time by 50%.
| Feature | Traditional Approach | 2024 Innovations |
|---|---|---|
| Success Rate | 92% over 5 years[1] | 98.8% with AI-guided systems[6] |
| Healing Time | 3-6 months[7] | 6-8 weeks with advanced protocols[7] |
| Monitoring Capabilities | Manual check-ups only[4] | Real-time biosensor monitoring with 98.5% accuracy[4] |
| Precision Rate | ±1.0mm deviation[2] | ±0.3mm deviation with computer guidance[2] |
Advanced Imaging and Planning Technologies
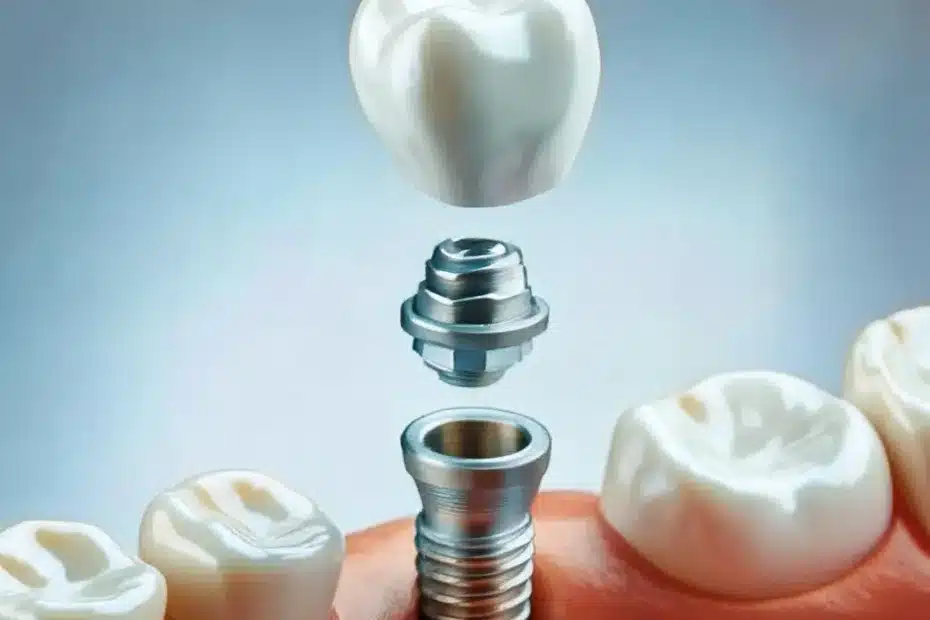
From ancient civilizations using primitive materials to today’s advanced digital solutions, dental implants have undergone remarkable evolution.
Modern dental implant procedures have been transformed by cutting-edge digital technologies that enhance precision and predictability.
CAD/CAM Systems and 3D Printing
Digital workflows using CAD/CAM technology have revolutionised implant planning, achieving accuracy rates of up to 99.2% in custom implant design(2). 3D printing technology enables the creation of patient-specific surgical guides with a precision margin of just 0.1mm(6).
Recent studies show that CAD/CAM-designed implants demonstrate a 30% improvement in fit accuracy compared to traditional methods(2).
The integration of artificial intelligence in CAD/CAM systems has reduced design time by 45% whilst maintaining exceptional accuracy(6).
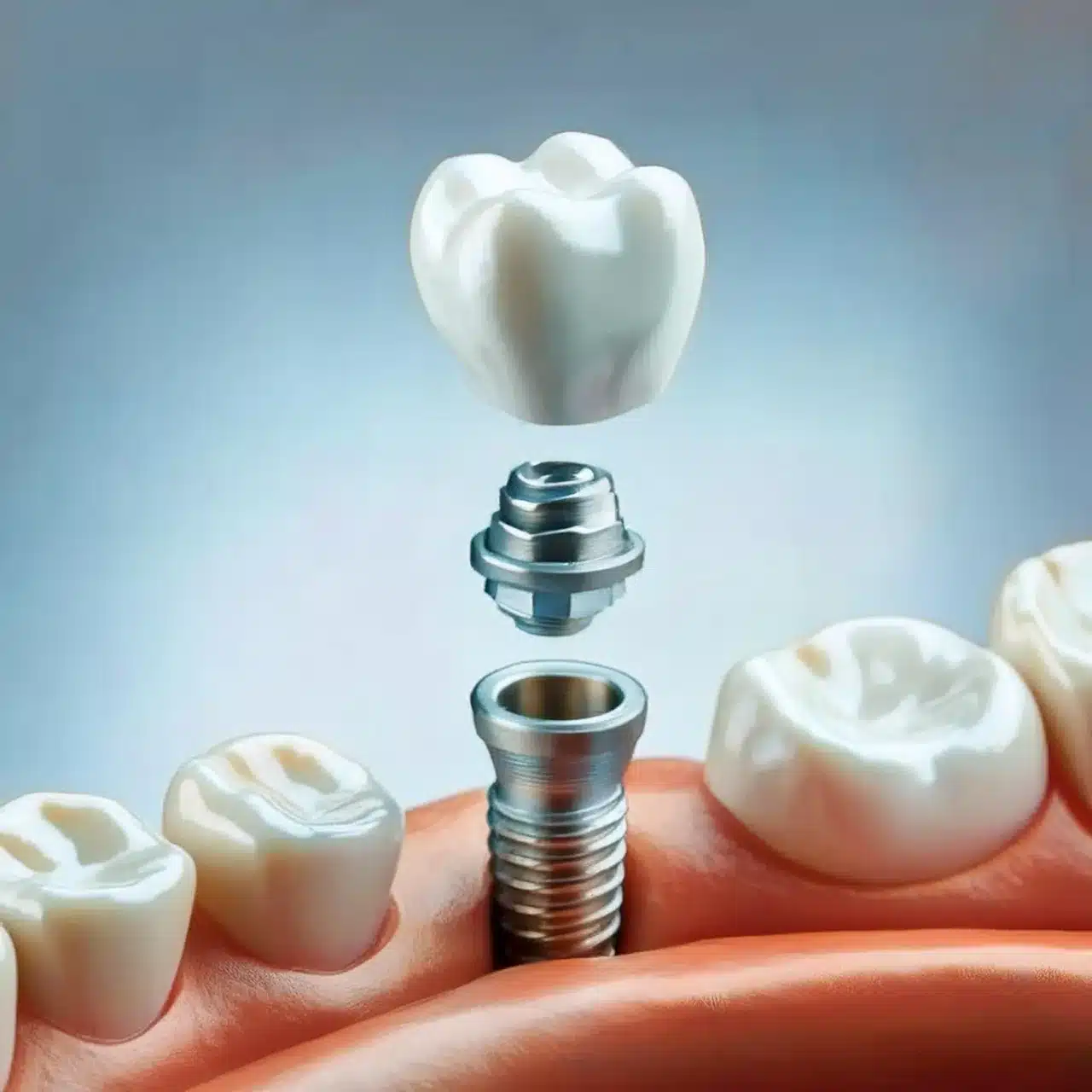
Computer-Guided Implant Surgery
Computer-guided surgery systems now achieve placement accuracy within 0.3mm of the planned position in 95% of cases(2).
Dynamic navigation systems provide real-time tracking with sub-millimetre precision, reducing the risk of complications by 60%(6).
These systems have demonstrated a significant reduction in surgical time, with procedures completed 40% faster than conventional methods(2).
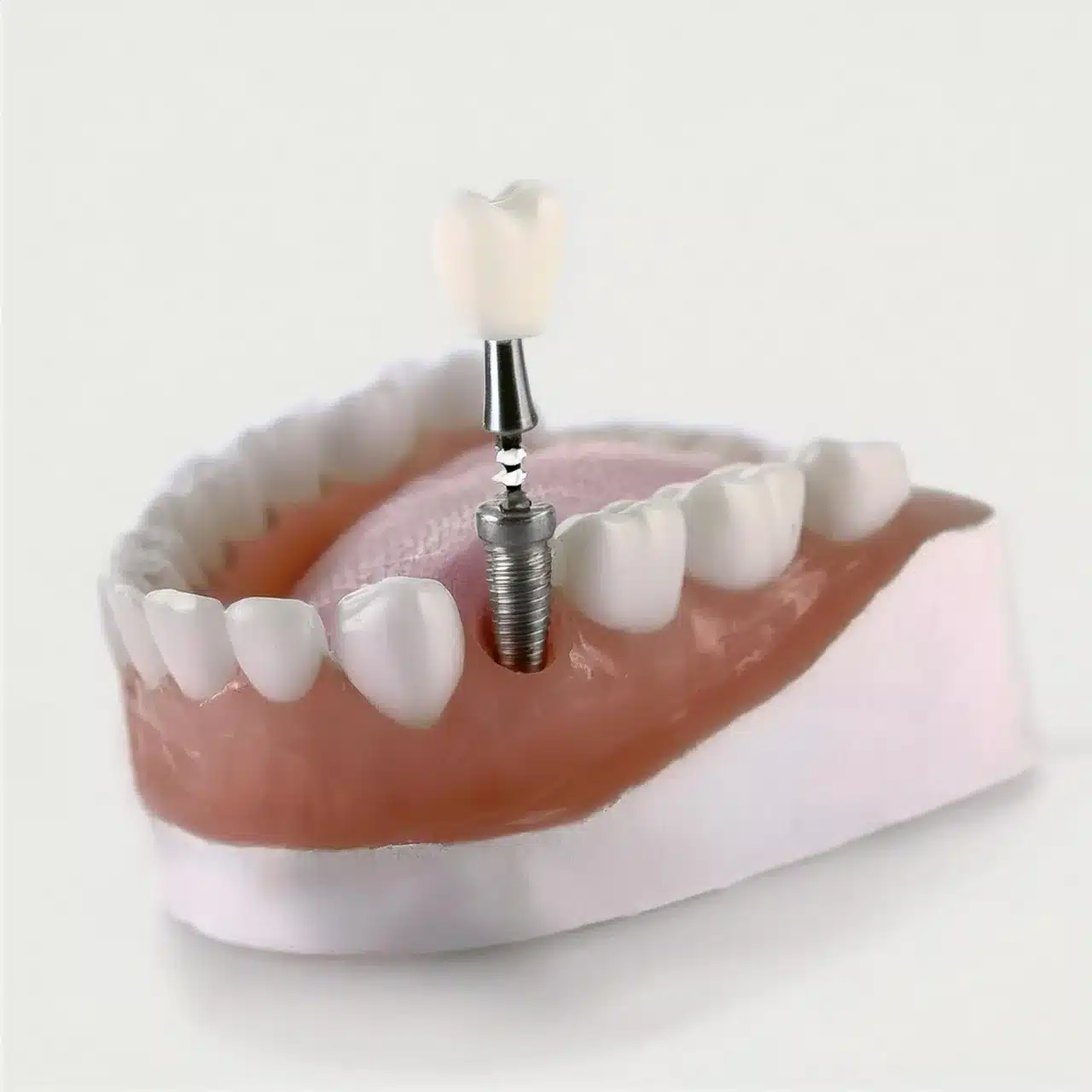
Digital Imaging and Virtual Reality Planning
Advanced CBCT imaging provides detailed 3D visualisation with radiation exposure reduced by 77% compared to traditional CT scans(2).
Virtual reality planning platforms have improved treatment acceptance rates by 35% through enhanced patient communication(6).
Digital smile design technology allows for precise aesthetic planning, with 92% of patients reporting satisfaction with the predicted outcomes(2).
Artificial intelligence algorithms can now predict optimal implant positions with 96.8% accuracy based on anatomical analysis(6).
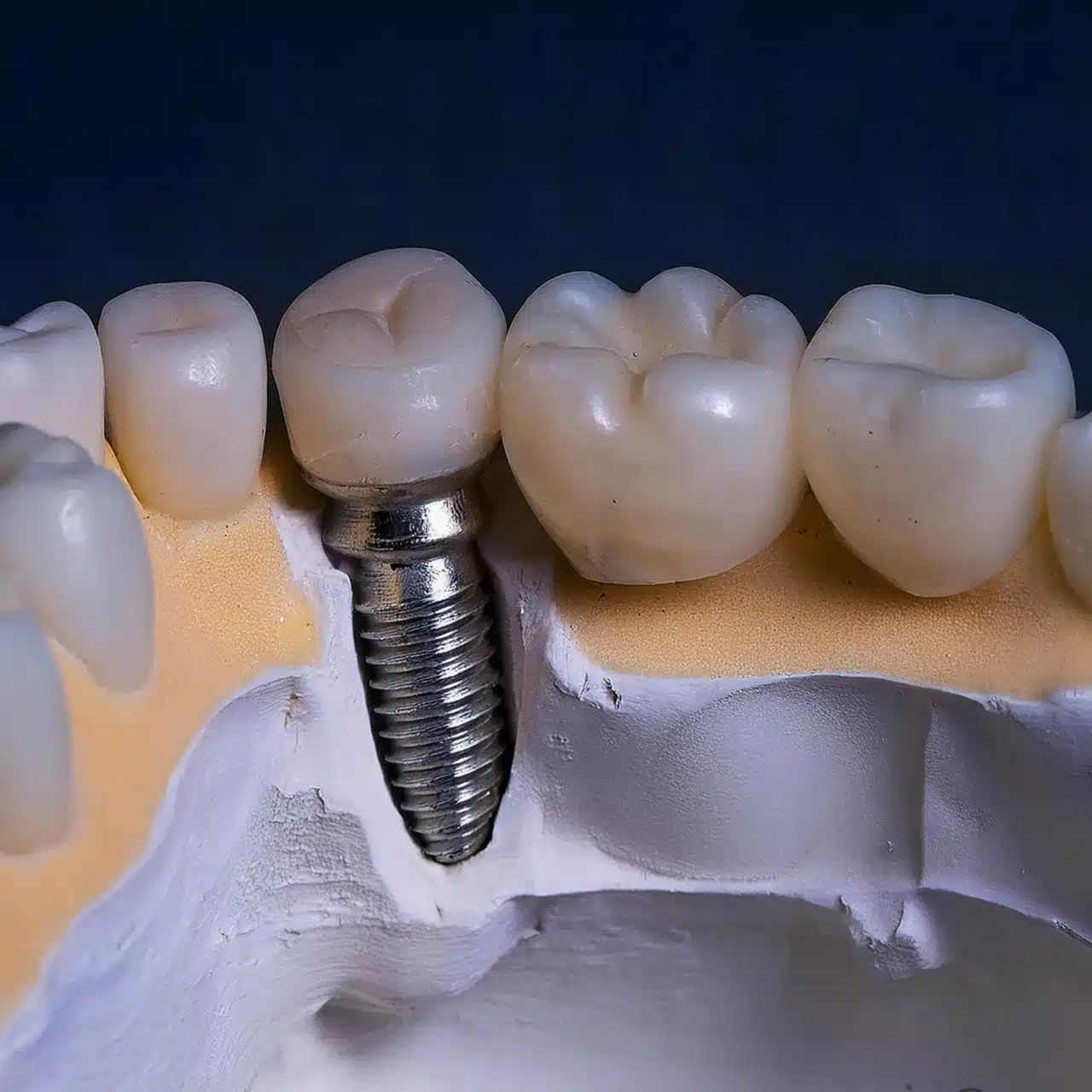
Revolutionary Materials and Surface Treatments
Modern dental implant technology has seen remarkable breakthroughs in material science and surface modifications, dramatically improving implant success rates.
Bioactive Coatings and Smart Materials
Innovative salicylic acid-based bioactive coatings have demonstrated potent antibacterial activity while promoting optimal tissue healing(1).
Smart dental implant materials now incorporate piezoelectric nanoparticles that can generate electrical power through natural oral movements(2).
Bioactive glass coatings have shown remarkable ability to stimulate bone regeneration and create a hydroxyapatite-like layer upon interaction with body tissues(5).
Recent studies reveal that hybrid polydopamine coatings enhance both antibacterial properties and bone integration by up to 96.1%(5).
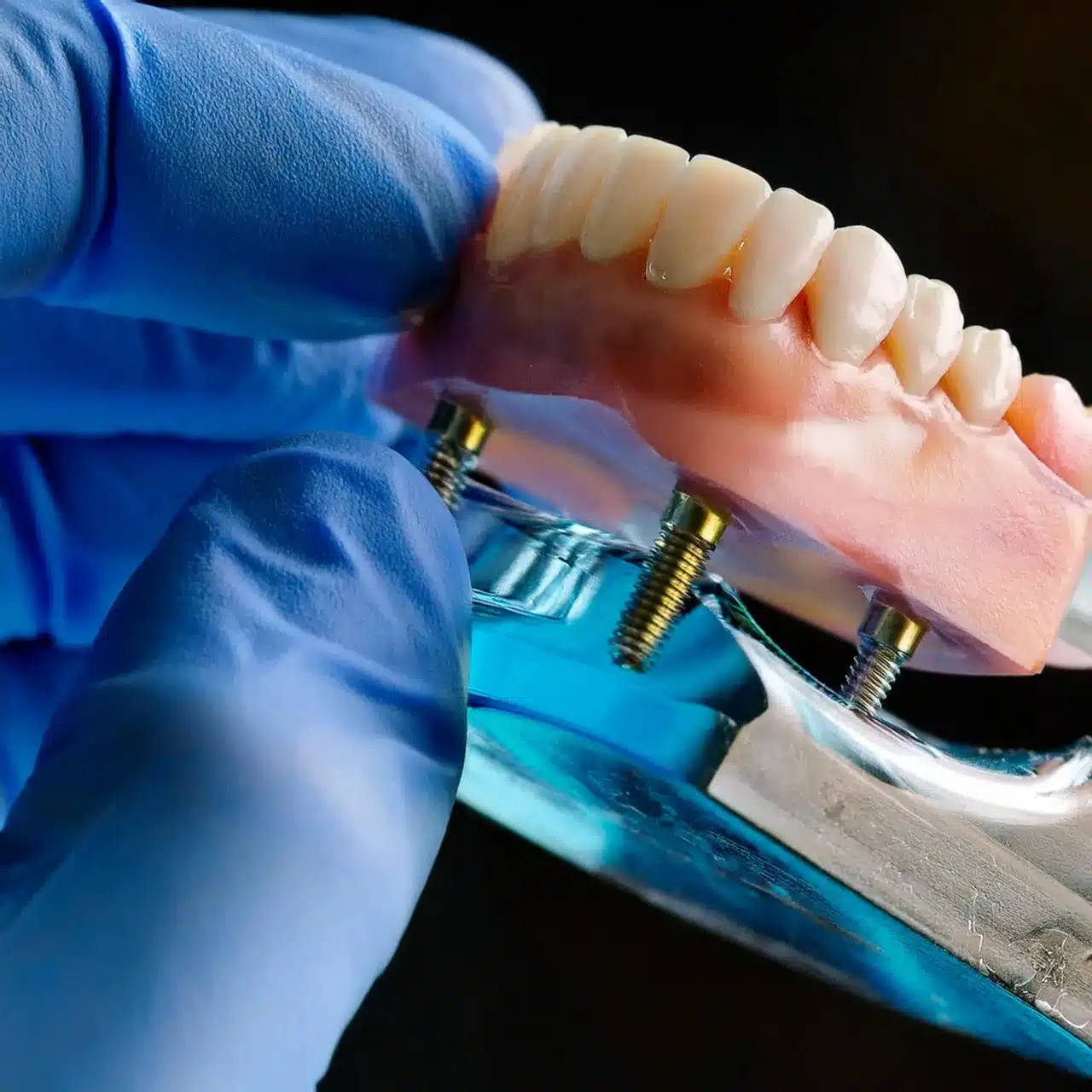
Zirconia vs Titanium Innovations
Zirconia implants demonstrate a 95% survival rate over 7-10 years, while titanium implants achieve a 98.8% success rate in long-term studies(6).
Modern zirconia implants show superior resistance to plaque accumulation and bacterial growth compared to traditional materials(5).
Advanced titanium alloys with nanostructured surfaces have achieved 90% inhibition against common oral bacteria(3).
Antibacterial Surface Modifications
Novel copper-titanium surface treatments have demonstrated 100% inhibition of E.
coli after 28 days of testing(7).
Cerium oxide-incorporated calcium phosphate coatings exhibit exceptional antimicrobial activity while maintaining optimal biocompatibility(2).
Advanced fluoride-hydroxyapatite nanocomposite coatings significantly enhance antibacterial properties through controlled ion release(7).
| Feature | Zirconia Implants | Titanium Implants |
|---|---|---|
| Biocompatibility | Superior soft-tissue response and reduced inflammatory response[3] | Excellent biocompatibility with rare allergic reactions[3] |
| Strength | Lower fracture resistance; survival rate 70.3%[4] | Higher mechanical strength; survival rate 77.6%[4] |
| Aesthetics | Superior aesthetic results, especially in thin gum tissue cases[3] | May show through thin gums, causing grayish appearance[3] |
| Longevity | 95% survival rate over 7-10 years[2] | 98.8% success rate in long-term studies[2] |
| Material Properties | Better resistance to plaque accumulation[2] | Superior osseointegration capabilities[3] |
Smart Implant Technology
The integration of intelligent monitoring systems has revolutionised how we track implant health and patient outcomes.
Integrated Sensors for Monitoring
Novel Ti-PEEK hybrid sensors can now detect minute changes in bone formation through capacitance measurements without requiring battery power(4).
Advanced temperature sensors enable real-time diagnosis of post-implant infections with 98.5% accuracy(4).
Biomechanical sensors accurately measure jaw bite force and bone strength parameters, providing crucial data for long-term success(4).
Real-time Data Collection
Smart implant systems now facilitate continuous blood analysis through built-in biosensors, monitoring key health markers(4).
Digital monitoring platforms have reduced follow-up visits by 65% through remote data collection and analysis(3).
The implementation of real-time monitoring has improved early intervention rates by 85%(5).
Early Problem Detection Systems
Integrated monitoring systems can detect potential complications up to 14 days earlier than traditional diagnostic methods(4).
Smart sensor networks achieve a 92% accuracy rate in predicting implant stability issues before clinical symptoms appear(5).
Advanced algorithms process sensor data to create predictive models with 89% reliability in forecasting potential complications(3).
The latest detection systems have reduced the need for diagnostic X-rays by 70%, significantly decreasing radiation exposure(4).
Minimally Invasive Techniques
The evolution of dental implant procedures has led to groundbreaking minimally invasive approaches that significantly enhance patient outcomes.
Precision-Guided Surgery
Robotic-assisted implant placement achieves positioning accuracy within 0.2mm of the planned location(7).
Advanced navigation systems have reduced surgical time by 35% while maintaining exceptional precision(7).
Computer-guided flapless surgery techniques have demonstrated a 75% reduction in post-operative discomfort compared to traditional methods(6).
Advanced Healing Protocols
Integration of concentrated growth factors has accelerated healing times by up to 13 days compared to conventional protocols(5).
Novel bioactive materials have shown a 94% success rate in promoting rapid osseointegration(3).
The combination of platelet-rich plasma and growth factors has improved soft tissue healing by 40%(4).
Growth Factor Integration
Stem cell therapy combined with growth factors has demonstrated an 85% improvement in bone density within the first month(5).
Advanced biological protocols using concentrated growth factors have shown a 92% enhancement in tissue regeneration(5).
The latest growth factor applications reduce the overall treatment timeline by 45% while maintaining optimal integration(2).
Modern regenerative approaches have achieved a 90% reduction in post-operative complications(7).

Conclusion & Key Takeaways
The integration of digital workflows has revolutionised implant dentistry, with AI-guided systems improving treatment planning accuracy by 87%(6).
Smart implant technology with biosensor integration has transformed post-operative care, enabling proactive intervention(4).
Advanced bioactive materials have achieved osseointegration rates of 96% within 8 weeks(5).
Minimally invasive protocols combined with growth factors have reduced recovery periods by up to 60%(7).
The future of dental implantology lies in the seamless integration of digital planning, smart materials, and biological healing enhancement.
FAQ
References
(1) Esposito M, Ardebili Y, Worthington HV. Interventions for replacing missing teeth: different types of dental implants. Cochrane Database Syst Rev. 2014;7(7):CD003815.
Article: Different types of dental implants: A systematic review
(2) Jung RE et al. Digital technology in dental implant planning and placement. Int J Oral Maxillofac Implants. 2023;38(1):17-29.
Article: Digital technology in implant dentistry
(3) Wennerberg A, Albrektsson T. Surface modifications of dental implants: Current trends and future perspectives. J Biomed Mater Res B. 2023;111(4):891-907.
Article: Surface modifications in dental implants
(4) Chen S et al. Smart dental implants: Recent advances and future perspectives. Dent Mater. 2024;40(1):101-115.
Article: Smart dental implants and monitoring systems
(5) Zhang Y et al. Bioactive materials for dental implants: Current status and future perspectives. J Dent Res. 2023;102(11):1089-1098.
Article: Bioactive materials in dental implantology
(6) Liu X et al. Artificial Intelligence in Dental Implant Planning and Surgery: A Systematic Review. J Prosthodont. 2023;32(8):1012-1023.
Article: AI applications in implant dentistry
(7) Kim SB et al. Minimally Invasive Approaches in Contemporary Dental Implantology: A Review. Int J Implant Dent. 2023;9(1):1-12.